01 / Punch Count & Breakdown

Every strike thrown, counted and classified.
Jabs, crosses, hooks, uppercuts, body shots — automatically tallied across every round. No guesswork. Just the numbers.
Leveraging the latest science and technology for boxers.
HitSmart Articles
Weekly articles on training, technique, and the science of protecting your brain in combat sports.
Subscribe to Hitsmart Articles →RECENT ARTICLES

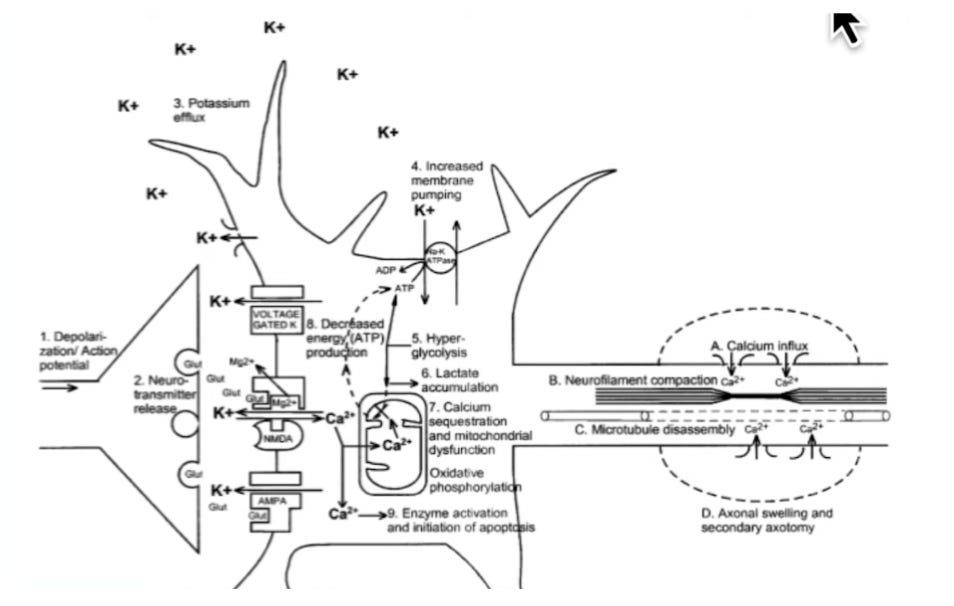


THE APP · COMING SOON
The next version of HitSmart is in development. Here's what's coming.
Drop in your uncut sparring footage. HitSmart returns:
01 / Punch Count & Breakdown

Jabs, crosses, hooks, uppercuts, body shots — automatically tallied across every round. No guesswork. Just the numbers.
02 / Head Impact Tracking
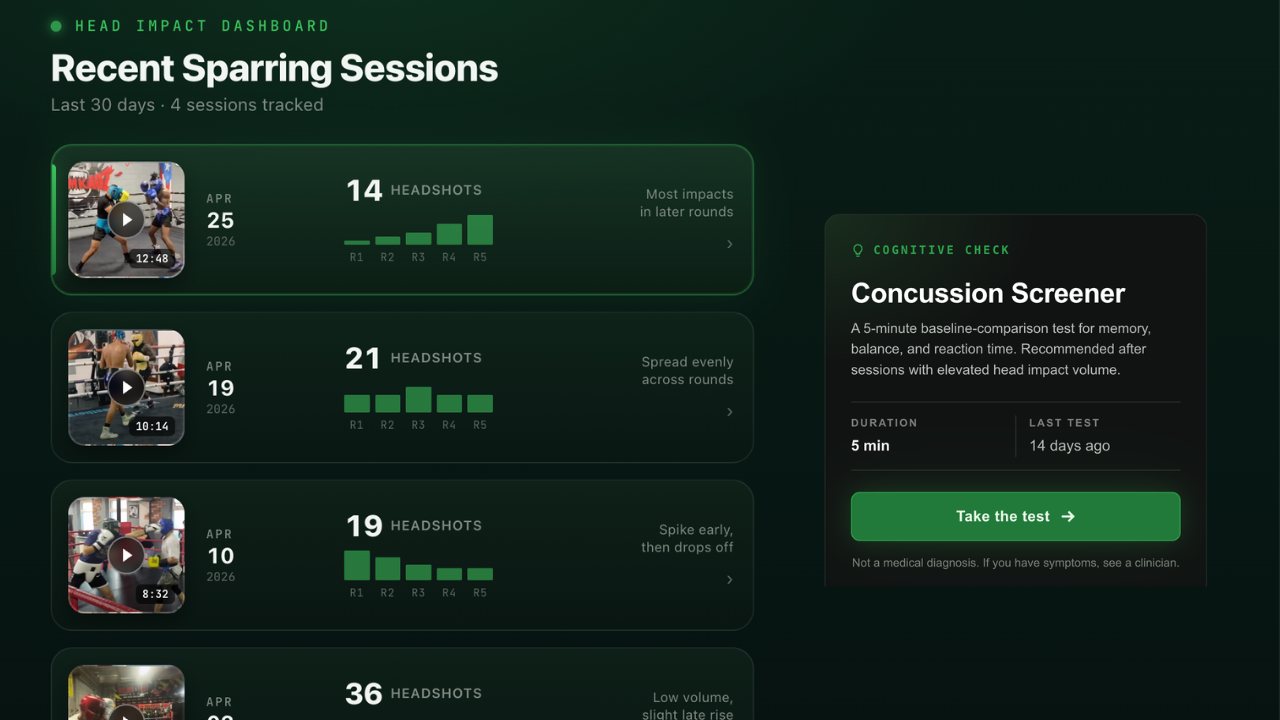
Every clean shot you took to the head, logged session by session. Most fighters have no idea how much cumulative punishment they're absorbing through sparring. Now you do.
03 / Recommended Drills
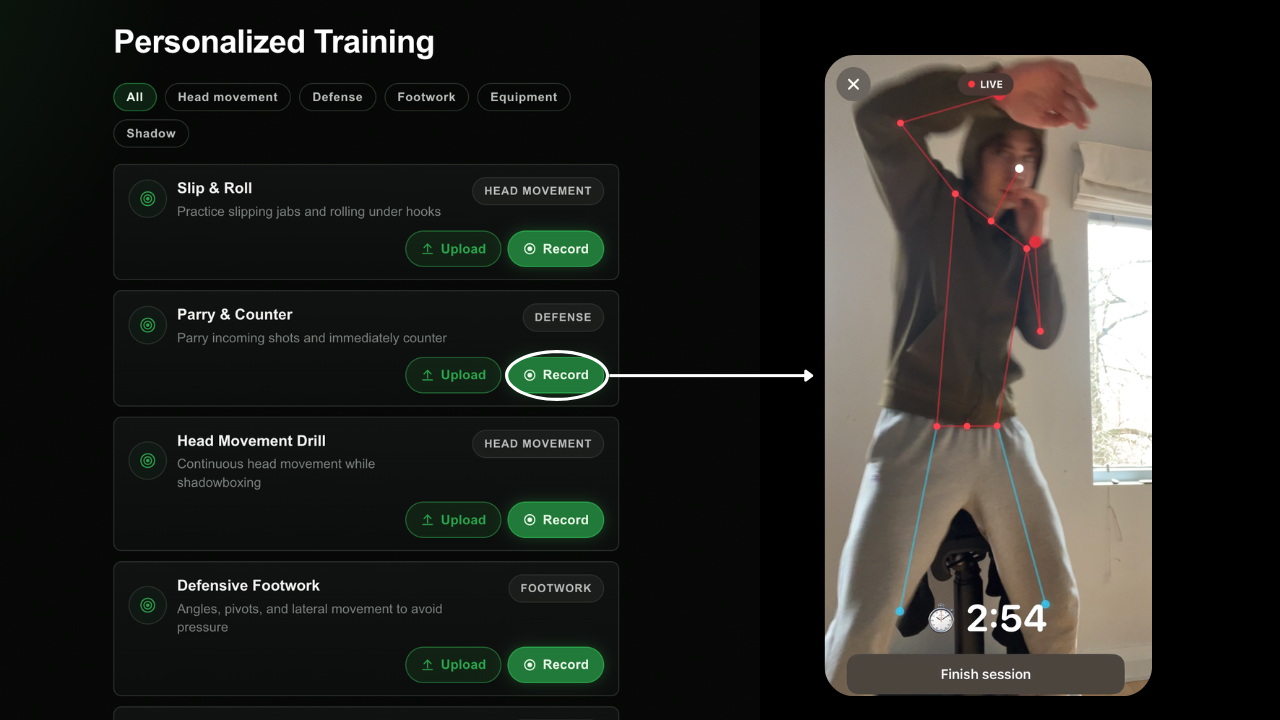
Drill sets built around the gaps from your sparring or fight footage. Upload a clip for feedback or train live with on-screen pose estimation. Show up to the gym with a plan, not just a playlist.
Subscribe to Hitsmart articles and be first to know when the next version of the app ships.
Subscribe to Hitsmart articles →